
In critical care settings, the importance of an ICU monitor cannot be overstated. These devices provide continuous and real-time data on vital signs, which is crucial for patient assessment and intervention. According to a recent report by the American Association of Critical-Care Nurses, timely monitoring can reduce mortality rates by up to 30% in acute care scenarios. This statistic underscores the life-saving capability of ICU monitors.
Dr. Emily Harris, a leading expert in critical care technology, emphasizes, “An ICU monitor is the lifeline for patients in critical conditions.” This statement reflects the consensus within the medical community on the necessity of these monitors. They track heart rate, blood pressure, oxygen saturation, and more, allowing healthcare providers to make informed decisions rapidly.
However, reliance on ICU monitors can lead to potential shortcomings. Data overload and sensor malfunction can complicate clinical judgments. It's essential for teams to strike a balance between relying on technology and exercising clinical expertise. Continuous training and evaluation are necessary to adapt to the challenges presented by these dynamic environments.
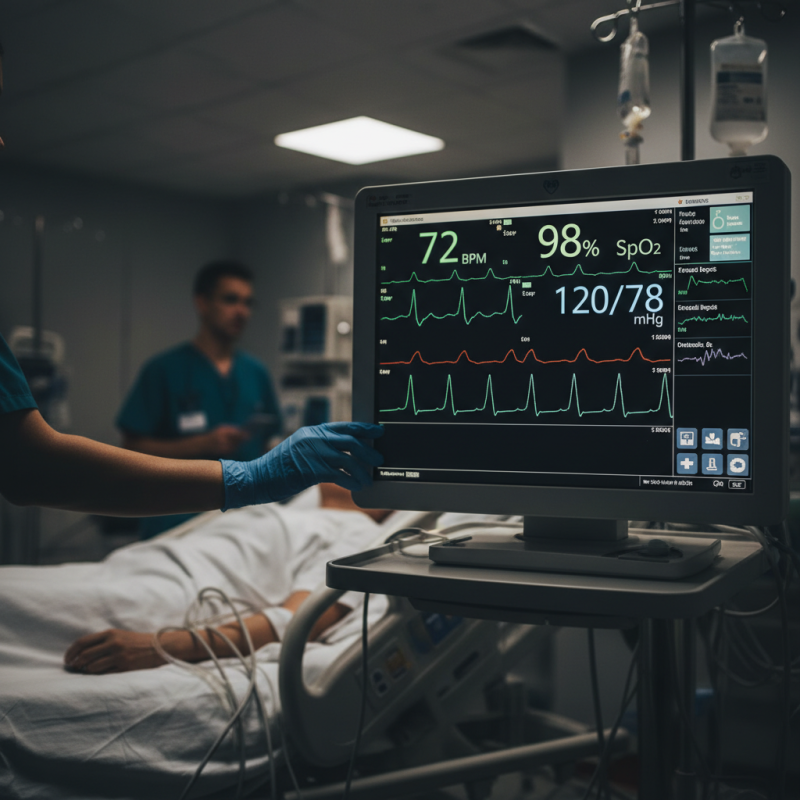

In critical care settings, ICU monitors play a pivotal role. They continuously track vital signs such as heart rate, blood pressure, and oxygen saturation. According to a 2022 report from the American Association for Critical Care Nurses, accurate monitoring can reduce adverse events by 25%. This statistic underscores the importance of vigilance in patient care.
ICU monitors also provide real-time data that guide clinical decision-making. They allow healthcare professionals to respond immediately to any changes. For instance, a sudden drop in blood pressure can indicate a life-threatening condition. However, despite advancements, there are still concerns about alarm fatigue. A study published in the Journal of Critical Care found that 80% of ICU staff often ignore monitor alarms due to their frequency. This raises questions about the effectiveness of monitoring systems.
Furthermore, the integration of advanced technology in ICU monitors offers richer data analysis. This can enhance diagnostic accuracy. However, the complexity introduces a learning curve for healthcare staff. The challenge lies in balancing technology with human intuition. While ICU monitors are essential, their efficacy heavily relies on skilled personnel to interpret the data.
In critical care environments, ICU monitors play a vital role. These devices track patients' vital signs continuously. They measure heart rate, blood pressure, and oxygen levels. This real-time data helps healthcare professionals make quick decisions. A sudden change in a patient’s condition can be life-threatening. Thus, timely alerts from monitors are crucial.
ICU monitors also display trends over time. This feature allows for in-depth analysis of a patient's health. Doctors may notice patterns that indicate improvement or deterioration. However, reliance on monitors can lead to overconfidence. Medical professionals must still use their clinical judgment. An alarming monitor doesn't always guarantee a problem exists.
Equipment calibration and regular maintenance are key to reliable readings. In some cases, monitors can produce false alarms. This can lead to alarm fatigue among staff. Misinterpretations sometimes occur, causing unnecessary worry. Vigilance is required to balance technology and human expertise, on which patient care depends.

In critical care settings, continuous monitoring is vital for improving patient outcomes. Research indicates that patients in ICU settings monitored continuously experience better survival rates. A study published in the "Journal of Critical Care" reveals that continuous monitoring can reduce the rate of adverse events by up to 30%. This highlights the essential role of ICU monitors in detecting complications early.
ICU monitors track vital signs and physiological changes in real-time. This allows healthcare providers to respond promptly to any deterioration in a patient's condition. For instance, when heart rates or oxygen levels fluctuate outside of normal ranges, clinicians can act swiftly, potentially saving lives. However, it's important to note that excessive reliance on monitoring technology can lead to alarm fatigue among staff, which may hinder response times.
Despite these challenges, the integration of advanced monitoring systems has proven effective. According to a report by the American Association of Critical-Care Nurses, regular assessments facilitated by monitoring tools can enhance decision-making efficiency by up to 40%. This demonstrates the power of continuous monitoring but also points to the need for regular staff training. Effective training ensures that providers can leverage the technology fully while minimizing the risk of information overload.
In critical care settings, ICU monitors are vital tools. They not only track vital signs but also provide real-time data to healthcare providers. Different types of monitors cater to various patient needs. For instance, multiparameter monitors measure heart rate, blood pressure, and oxygen saturation. Some advanced units also integrate capnography, offering insights into a patient's ventilation status. A report from Frost & Sullivan highlighted that the global market for ICU monitoring systems is expected to reach $6.1 billion by 2025, underscoring their critical role in patient care.
Bedside monitors are commonly used in ICU environments. They can alert staff to sudden changes in a patient’s condition, which is crucial for timely interventions. However, not all monitors are created equal. Some lack specific features or accuracy. A study by the American Journal of Critical Care noted that 30% of alarms were false, causing alarm fatigue among staff. This reflects the need for continuous improvement in monitor technology. Advanced forms use artificial intelligence to reduce false alarms, but they are not universally available yet and require careful assessment.
Remote monitoring systems are gaining traction. They provide data to off-site specialists, enhancing patient evaluation during critical moments. Despite their benefits, reliance on technology can be problematic. Missed alarms and data overload remain concerns. Healthcare providers must balance technology use with clinical judgment to ensure optimal patient outcomes. This is an ongoing challenge in the evolution of ICU care.
In critical care settings, ICU monitors play a crucial role. They continuously track vital signs like heart rate, blood pressure, and oxygen saturation. However, these sophisticated devices come with their own set of challenges. One significant issue is the potential for alarm fatigue among healthcare providers. Constant beeping can lead to desensitization, making it easier to overlook important alerts. This can jeopardize patient safety.
Another limitation lies in the accuracy of the data collected. Monitors may produce false readings due to a variety of factors, such as motion artifacts or poor sensor placement. This can lead to misinterpretations of a patient’s condition. Additionally, not all monitors are equipped with advanced analytics, which can hinder timely decision-making. There can be gaps in data integration, making it challenging to get a complete picture of a patient's health.
Moreover, dependence on technology can create a false sense of security. Healthcare professionals must remain vigilant and not rely solely on monitors for clinical assessments. Continuous training and awareness about the limitations of these devices are necessary. While ICU monitoring technology is a vital part of patient care, it is essential to understand its shortcomings to ensure comprehensive and reliable treatment.





©2026Infinium Medical
Adding {{itemName}} to cart
Added {{itemName}} to cart