
The landscape of healthcare is rapidly changing, driven by technology. The demand for remote patient monitoring equipment has surged, particularly due to the COVID-19 pandemic. A recent report from the Global Market Insights indicates a growth rate of over 30% for the remote patient monitoring market by 2026. This statistic underscores the increasing reliance on telehealth solutions.
Choosing the right remote patient monitoring equipment is crucial for delivering effective care. Many healthcare providers now face overwhelming options. Providers must consider factors such as device reliability, ease of use, and data security. For instance, a study published in the Journal of Medical Internet Research highlighted that 41% of patients prefer devices that integrate with existing health applications. However, not all devices measure up to these expectations.
It is essential to reflect on the long-term impact of these tools. While they can improve patient outcomes, some devices may not provide accurate data. Poorly selected monitoring equipment can lead to mismanagement of care. Therefore, healthcare professionals must diligently assess each option. The goal is to enhance patient engagement and ensure safety through effective remote monitoring strategies.

Remote Patient Monitoring (RPM) is transforming healthcare delivery. It allows providers to track patients’ health data in real-time. This is particularly crucial for managing chronic illnesses. According to a recent report, RPM can reduce hospital readmission rates by up to 30%. This can significantly lessen healthcare costs.
However, adopting RPM systems is not without challenges. Many healthcare providers struggle with choosing the right equipment. The available options can be overwhelming. Devices must be user-friendly for both patients and providers. A study showed that 40% of patients found technical issues difficult to manage. Clearly, usability is key.
Furthermore, data security remains a major concern. With increasing data breaches, ensuring patient privacy is crucial. A report indicated that around 30% of healthcare organizations faced cyber threats. Patients must trust that their data is safe. This trust is essential for RPM success. Investing time in understanding these factors can drive effective RPM implementations.
| Equipment Type | Key Features | Patient Suitability | Data Transmission | Cost Range ($) |
|---|---|---|---|---|
| Blood Pressure Monitor | Automated readings, Bluetooth connectivity | Hypertension patients | Bluetooth, Wi-Fi | 50 - 150 |
| Pulse Oximeter | Real-time oxygen saturation monitoring | Patients with respiratory issues | Bluetooth, USB | 20 - 60 |
| Weight Scale | BMI calculation, smart notifications | Obesity management | Wi-Fi, Bluetooth | 30 - 100 |
| Glucose Monitor | Continuous glucose monitoring, alerts | Diabetes patients | Bluetooth, Mobile app | 50 - 300 |
| Heart Rate Monitor | ECG, real-time data sharing | Cardiac patients | Bluetooth, Wi-Fi | 70 - 250 |
When selecting remote patient monitoring (RPM) equipment, several factors are vital for effective care. One key factor is the usability of the device. It must have an intuitive interface, easy enough for patients of all ages. If patients struggle to operate the device, data accuracy can be compromised. Look for simple setup procedures and clear instructions. This enhances compliance and maximizes the utility of the technology.
Another significant aspect is the type of data the equipment captures. Ensure that it aligns with the specific needs of your patient population. For example, if monitoring chronic conditions, devices must accurately track vital signs like heart rate or blood pressure. The device should also provide real-time alerts, enabling timely intervention. However, consider the potential overwhelming nature of constant updates. Balancing the frequency of notifications can prevent alert fatigue among users.
Additionally, compatibility with existing health IT systems is crucial. The equipment should seamlessly integrate with electronic health records (EHRs). This interoperability ensures that data collected is easily accessible for healthcare providers. Still, assess whether your current systems can adapt to new technology. Transitioning to new platforms can be challenging and may cause temporary data disconnects. Remember, selecting RPM equipment is a thoughtful process that requires ongoing evaluation and reflection.
When selecting remote patient monitoring devices, it’s vital to understand the types available. Each type serves a distinct purpose in managing patient health effectively. Common devices include blood pressure monitors, glucose meters, and heart rate trackers. These tools collect essential health data from patients in their homes.
Tips: Ensure you choose devices that are user-friendly. Complicated setups may deter use. A simple interface encourages consistent monitoring and engagement. Battery life is also crucial; constant charging can be inconvenient.
Consider the integration of these devices with health apps. Some devices sync health data to mobile platforms, allowing for easier tracking. This feature can enhance communication between patients and healthcare providers. Reflect on what data is most relevant for your needs.
It's important to remember that not every device works for everyone. Some patients may feel overwhelmed by technology. Personal experience matters when choosing the right device. Testing out devices may lead to better choices for effective care.
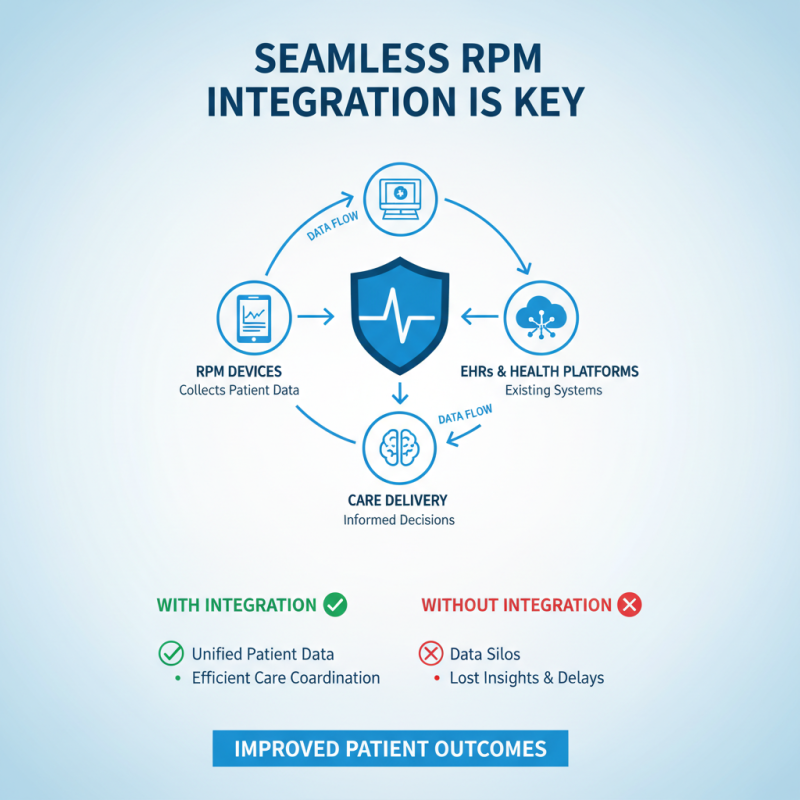
When choosing remote patient monitoring (RPM) equipment, integration is crucial. Compatibility with existing systems can make or break effective care delivery. Healthcare providers often struggle with data silos. RPM devices should easily connect to electronic health records (EHRs) and other health management frameworks. If they don’t, valuable data will be lost or isolated.
The integration process requires careful evaluation. Each device needs to share information seamlessly. For example, blood pressure monitors should transmit readings directly to the patient’s health record. Inconsistent data from disparate sources complicates patient monitoring. Moreover, clinical workflows should not be disrupted. Sometimes, implementing a new device ends up confusing staff and patients alike.
Testing compatibility early is key. Ensure that technical specifications align with current systems. Trials can reveal hidden issues before full deployment. Feedback from end-users is invaluable. While we aim for smooth integration, the reality may involve unexpected hurdles. Reflecting on these challenges can spark continuous improvement in RPM strategies.
When choosing remote patient monitoring (RPM) equipment, security and compliance are paramount. Patients share sensitive information. Any breach can lead to dire consequences. Therefore, evaluating the security measures of RPM technologies is crucial. Look for features like data encryption and user authentication. These safeguards help protect patient data from unauthorized access.
Compliance with regulations is another critical aspect. RPM tools must adhere to local and international privacy standards. Failure to do so can result in legal troubles. It's essential to review the documentation of equipment. Often, these documents reveal a company's commitment to compliance. However, not all manufacturers provide clear information. This gap creates uncertainty. Practitioners must ask questions and seek clarifications.
Another key point is usability. Even secure devices can be ineffective if they are complicated. Frontline healthcare workers need to understand the technology quickly. Systems should have intuitive interfaces. A device may be secure but hard to use. This can frustrate both patients and providers. Balancing security, compliance, and usability is a challenge. Constant reassessment is necessary to ensure effective care.





©2026Infinium Medical
Adding {{itemName}} to cart
Added {{itemName}} to cart